Tea tree oil got pigeonholed somewhere around 2005. It became “the acne thing.” But the same compound that fights acne bacteria - terpinen-4-ol from Melaleuca alternifolia - also reduces chronic low-grade inflammation, kills microscopic mites living in your pores, and speeds wound healing. These are not teenage skin problems. They matter profoundly after 45.
1. Terpinen-4-ol: The Compound That Makes Tea Tree Oil Actually Work
Tea tree oil is a complex essential oil containing over 100 identified chemical components, but its therapeutic activity is primarily driven by one monoterpene alcohol: terpinen-4-ol. This is the compound responsible for the antimicrobial, anti-inflammatory, and wound-healing effects that have been documented in clinical literature since the 1990s.
Terpinen-4-ol works through multiple mechanisms simultaneously. Against bacteria, it disrupts cell membrane integrity, causing cytoplasmic leakage and cell death. This mechanism works against both gram-positive organisms (like Staphylococcus aureus, the primary pathogen in infected skin wounds and eczema) and gram-negative organisms. Against Demodex mites, it appears to act as a neurotoxin, paralyzing and killing the mites at concentrations achievable with a properly diluted topical application.
Against inflammatory pathways, terpinen-4-ol suppresses lipopolysaccharide-induced production of TNF-alpha, IL-1beta, and IL-10 in monocytes - the exact inflammatory mediators that drive the chronic, low-grade inflammation (inflammaging) that accelerates collagen breakdown after estrogen declines. This makes tea tree oil relevant not just for acute skin conditions but for the day-to-day inflammatory burden of mature skin.
The practical takeaway: tea tree oil quality varies enormously. An oil with 20% terpinen-4-ol will not produce the same outcomes as one with 38%. Always choose tea tree oil that specifies its terpinen-4-ol content, ideally with a batch-level CoA. The ISO 4730 standard sets the floor at 30%, but higher is meaningfully better for therapeutic use.
2. Demodex Mites and Rosacea-Like Redness (the Connection Nobody Talks About)
Demodex folliculorum and Demodex brevis are microscopic mites that live in hair follicles and sebaceous glands. Every adult human has them. That is normal. What becomes problematic after 45 is population density - and the disruption in immune regulation that comes with declining estrogen allows Demodex populations to overgrow in a significant proportion of women in this age group.
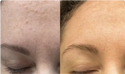
Overgrown Demodex populations cause a constellation of symptoms that are routinely misdiagnosed or attributed to rosacea: persistent redness, a sensation of crawling or itching on the skin (especially at night when mites are most active), follicular papules, and rough skin texture despite adequate moisturization. The redness is not vascular - it is inflammatory, driven by the mites’ waste products and the immune response they trigger.
Terpinen-4-ol is one of the few topical agents with documented efficacy against Demodex. A 4-week study using a 5% tea tree oil scrub and 50% tea tree oil eyelid treatment significantly reduced mite density and symptom scores in patients with Demodex-associated blepharitis - a condition directly analogous to Demodex overgrowth in facial follicles.
If you have been diagnosed with rosacea that does not respond to standard treatments, or if your skin experiences burning or itching most prominently at night, Demodex overgrowth is worth investigating. A dermatologist can perform a skin scraping to confirm. If confirmed, a properly diluted tea tree oil protocol applied nightly is an evidence-backed treatment option.
3. Calming Chronic Inflammation and Sensitive Skin
The distinction between acute inflammation (redness from a pimple) and chronic low-grade inflammation (the persistent background inflammatory state of post-menopausal skin) is critical for understanding where tea tree oil fits in a mature skincare routine.
Chronic low-grade inflammation in mature skin is not always visible. It does not always produce redness you can see. What it does, consistently, is activate matrix metalloproteinases - the enzymes that break down collagen and elastin. It also impairs the skin’s ability to repair damage from UV exposure, delays wound healing, and increases transepidermal water loss by disrupting tight junction protein expression in the epidermis.
Tea tree oil’s terpinen-4-ol reduces prostaglandin E2 production and inhibits histamine release from mast cells - two key mediators of the inflammatory response in skin. For women whose skin has become more reactive and sensitive since perimenopause, this represents a meaningful mechanism. The goal is not to suppress the immune response entirely but to moderate the chronic overactivation that characterizes inflammaging.
A 2020 study published in Molecules demonstrated that terpinen-4-ol at 0.1–0.5% concentrations significantly reduced inflammatory cytokine production in keratinocytes without cytotoxic effects on the cells. This is within the range achievable with a properly diluted topical preparation, confirming that anti-inflammatory effects do not require high concentrations.
4. Wound Healing When Your Skin Takes Longer to Recover
One of the less-discussed changes in skin after 50 is the measurable slowing of wound healing. The cellular mechanisms are well-documented: reduced fibroblast activity, lower TGF-beta signaling, decreased keratinocyte migration, and impaired angiogenesis (new blood vessel formation) at wound sites. A cut that healed in a week at 30 may take two to three weeks at 55. Minor irritation that would have resolved overnight can linger for days.
Tea tree oil influences wound healing through two mechanisms. First, its antimicrobial activity reduces the bacterial burden at wound sites, which is the primary cause of delayed healing in mature skin. Second, terpinen-4-ol has been shown in vitro to stimulate fibroblast activity and keratinocyte migration - both essential for re-epithelialization of wound sites.
A 2013 study by Chin and Cordell demonstrated significantly faster wound closure in tea tree oil-treated wounds compared to controls in an in vitro model. A subsequent human study found that a tea tree oil preparation reduced healing time for minor excisions and skin trauma compared to standard antiseptic treatment.
The clinical application: a 1% tea tree oil preparation applied to minor skin wounds, small cysts after extraction, or post-procedure sites (with physician clearance) may meaningfully accelerate the slower healing timeline mature skin presents.
5. Hormonal Breakouts During Perimenopause (Yes, It Happens)
Perimenopause does not produce the kind of acne you had at 17. What it produces is typically cystic, deep-set breakouts concentrated along the jawline and lower face, driven by the relative androgen excess that occurs as estrogen declines faster than testosterone in the perimenopausal transition. Sebum production becomes dysregulated, follicles are more prone to becoming blocked, and the bacteria that colonize blocked follicles - primarily Cutibacterium acnes (formerly Propionibacterium acnes) - have more material to work with.
Tea tree oil’s efficacy against C. acnes is among the most consistently replicated findings in the tea tree literature. A landmark 1990 randomized controlled trial by Bassett et al. found that 5% tea tree oil gel produced equivalent reductions in lesion counts to 5% benzoyl peroxide gel over 12 weeks, with significantly fewer side effects - less dryness, less irritation. For mature skin that cannot tolerate the barrier disruption of high-concentration benzoyl peroxide, this is a meaningful alternative.
The application method matters for perimenopausal breakouts. Spot treatment with a 2–5% tea tree oil preparation applied directly to forming lesions at their first appearance (the inflamed stage, before a visible head forms) is more effective than general facial application. Mature skin cannot tolerate the drying effect of broad tea tree application - concentrated spot use preserves the barrier everywhere else.
6. Eczema and Stubborn Dry Patches That Won’t Respond to Moisturizer
Atopic dermatitis (eczema) and its milder presentations - localized dry patches, contact dermatitis flares, winter-pattern xerosis - become more common after menopause. The mechanisms are interconnected: declining ceramide production weakens the stratum corneum’s barrier function, allowing irritants and allergens to penetrate more easily, triggering immune responses that produce the characteristic inflammation and itch cycle.
Staphylococcus aureus colonization of eczematous skin is a significant driver of flare severity. In eczema, the bacterial burden of S. aureus on affected skin is 100 to 1,000 times higher than on normal skin. Tea tree oil’s demonstrated efficacy against S. aureus - including methicillin-resistant strains (MRSA) at higher concentrations - makes it relevant to the management of eczema flares.
A 2011 study comparing tea tree oil, zinc oxide, and clobetasone butyrate (a topical steroid) in the treatment of eczema found that tea tree oil was significantly more effective than zinc oxide and not significantly different from the steroid for reducing overall severity scores, but with a substantially more favorable side effect profile for long-term use.
The dilution protocol for eczematous skin is conservative: 1% in a fatty carrier oil applied to affected areas only, not the full face, twice daily during flares. Do not exceed 2% on eczematous skin - higher concentrations can paradoxically increase irritation in already-compromised skin.
7. Antioxidant Protection for Sun-Damaged Mature Skin
Tea tree oil is not primarily known as an antioxidant ingredient, but its terpene compounds - including alpha-terpineol, gamma-terpinene, and p-cymene - contribute measurable free radical scavenging activity. More relevantly for mature skin, terpinen-4-ol has been shown to upregulate endogenous antioxidant enzyme expression in keratinocytes, specifically superoxide dismutase (SOD) and catalase.
This is significant because mature skin’s primary antioxidant challenge is not exogenous antioxidants in skincare products (though those help) - it is the declining capacity of the skin’s own enzymatic antioxidant systems. After menopause, keratinocyte SOD activity declines, leaving the skin more vulnerable to oxidative damage from UV exposure, pollution, and the normal metabolic activity of skin cells.
By upregulating SOD and catalase rather than simply applying exogenous antioxidants, tea tree oil compounds work with the skin’s existing biology rather than substituting for it. This complementary mechanism makes it a useful addition to an antioxidant-forward routine that might include vitamin C serum and carotenoid-rich botanical oils.
8. How to Use Tea Tree Oil Safely on Mature Skin (Dilution, Carriers, and Routine Layering)
The safety of tea tree oil on mature skin is entirely a function of proper dilution and application method. Undiluted tea tree oil applied to facial skin will cause chemical burns, contact dermatitis, and lasting sensitization. This is not hyperbole - it is a documented adverse effect that results in a permanently sensitized reaction to the ingredient. The good news is that at correct dilutions, tea tree oil is safe for mature skin including sensitive and reactive skin types.
Dilution for Mature Skin
Dilution calculation: 1% dilution = 6 drops of essential oil per 30ml (1oz) of carrier. 2% dilution = 12 drops per 30ml. 3% dilution = 18 drops per 30ml. For spot treatment rather than broad application, you can mix 1 drop of tea tree oil with 1 teaspoon of carrier oil for a roughly 1% preparation.
Start with 1% applied to a small test area on your inner forearm for 48 hours before applying to the face. This patch test protocol is not optional for mature skin - sensitivity to tea tree oil is dose-dependent, and establishing that you do not have a pre-existing sensitivity before facial application is important.
Build slowly: begin with three applications per week and increase to nightly use over two weeks if no irritation develops.
Carrier Oils for Women 45+
Not all carrier oils are equally appropriate for mature skin. For tea tree oil dilution, the carrier does dual work: it dilutes the essential oil to a safe concentration AND delivers its own skin benefits. The best choices for women 45+:
- Jojoba oil: wax ester structure closely mimics sebum; non-comedogenic; excellent for combination or acne-prone mature skin
- Rosehip oil: rich in linoleic acid and provitamin A; supports cellular turnover; ideal for hyperpigmentation and fine lines
- Sea buckthorn oil (1–3% in a lighter carrier): extreme carotenoid and omega-7 content; synergistic with tea tree for barrier repair
- Squalane: stable, lightweight, non-comedogenic; excellent base for spot treatments that need to absorb quickly
Avoid coconut oil as a carrier for facial use in mature skin: it is comedogenic for most people and the occlusive effect can trap the essential oil compounds against the skin at irritating concentrations.
Routine Layering
Tea tree oil preparations fit best in the treatment step of an evening routine, after cleansing and toning but before heavier oils and moisturizers:
- Cleanse
- Tone (if using)
- Water-based actives (vitamin C, niacinamide, hyaluronic acid serums)
- Tea tree oil preparation (spot treatment or diluted in carrier)
- Heavier facial oil or moisturizer
Niacinamide and peptides are fully compatible with tea tree oil on the same night. Do not use tea tree oil on the same night as retinol - alternate evenings to avoid compounding barrier disruption.

100% botanical actives. Sea buckthorn as the foundation. Zero water, zero synthetic preservatives. Rated 4.66/5 from 3,152+ reviews. 60-day money-back guarantee.
Shop the System - $119Precautions Specific to Mature Skin
Oxidation: Tea tree oil oxidizes with exposure to air, light, and heat. Oxidized tea tree oil becomes a distinct allergen - it no longer behaves the same way as fresh oil and can trigger sensitization reactions even in people who have previously tolerated it well. Replace your tea tree oil every 12 months regardless of how much remains. Store in dark glass, tightly capped, away from heat and light. If it develops a sharper, more chemical smell or darkens in color, it has oxidized - discard it.
Wound application: Do not apply tea tree oil to deep wounds, puncture wounds, or surgical incisions without physician guidance. For minor surface wounds, cuts, and post-extraction sites, 1% is appropriate.
Hormone-sensitive conditions: Some research suggests tea tree oil may have weak estrogenic and antiandrogenic activity. The evidence is from in vitro studies and the clinical significance for topical use at 1–2% is unclear. Women with hormone-sensitive conditions (certain breast cancers, endometriosis) should discuss with their physician before adding tea tree oil to their routine.