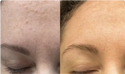
If your skin started flushing, burning, or breaking out in tiny bumps in your mid-40s and nothing you used to trust is working, you are not imagining it. The moisturizer that felt like a friend is suddenly stinging. The serum you have used for a decade leaves your cheeks blotchy by noon.
Most rosacea articles hand you a recycled kitchen-ingredient list. Raw honey. Green tea compresses. A vague warning about spicy food. None of them explain why your skin became reactive now, in this decade, after 45 calm years.
This piece does something different. I will walk you through the inflammation cascade in plain English, show you the hormonal connection almost no one is writing about, and rank natural rosacea treatment options by actual evidence. You will see which ingredients have human trial data, which have strong mechanisms but no rosacea-specific RCTs, and which are tradition wearing a lab coat. You will get a real routine, not a list.
Start with the part of the story almost nobody is telling you.
Why Rosacea Gets Worse in Perimenopause and Menopause
Estrogen has protected your skin from inflammation for decades, and most women have no idea until it leaves.
Estradiol does quiet daily work inside your skin. It regulates antioxidant enzyme activity. It suppresses NF-kB, the master switch that flips on almost every inflammatory gene in the body. It keeps oxidative stress in check. When estrogen drops in perimenopause, those brakes loosen at once, and skin that never flushed before starts to flush easily.
The research is not subtle. A West China Hospital study of 59 women (mean age 48.42) found estradiol was negatively correlated with erythematotelangiectatic rosacea severity (r=−0.021, p=0.005). Women with mild ETR had a mean estradiol of 95.82 pg/mL. Women with severe ETR had less than half, 42.28 pg/mL. That gap is not random.
A shared vascular pathway explains the pattern. Menopausal hot flashes and rosacea flushing both rely on prostaglandin-driven vasodilation. Each flush trains the facial vasculature to flush more readily next time. Over months, that becomes a progressive sensitization loop.
The emotional toll is documented. In the same study, 45.8% of women had anxiety and 40% met criteria for depression. What you are feeling is common and biological, not a personal failing.
Hormonal reality does not make you powerless. It means your treatment plan must differ from one you would have built at 30. To treat this, you need to understand what happens under the surface when your cheeks flush.
What Is Actually Happening Under Your Skin When You Flush
Your rosacea flush is not random. A specific chain of events fires in your skin in the 30 seconds before your cheeks turn red, and almost no article walks you through it.
It starts with the barrier. Rosacea-prone skin has a leakier, thinner stratum corneum. That is both cause and consequence. A weaker barrier lets irritants in and water out, priming the cascade.
Next comes the mite. Everyone has Demodex mites on their face. Rosacea skin has more of them, and the chitin in their exoskeletons activates TLR2 on your skin cells. That activation overdrives KLK5 (kallikrein-5), which cleaves cathelicidin into abnormally high amounts of a fragment called LL-37.
At normal levels, LL-37 is antimicrobial and helpful. At elevated levels, it flips pro-inflammatory and activates TRPV1, the same nerve channel that responds to heat, spice, and capsaicin. That is your neurogenic flush, your face going hot in under a minute.
A second pathway runs in parallel. The NLRP3 inflammasome activates, releasing IL-1beta and IL-18. Those cytokines drive the papules and pustules of papulopustular rosacea. Flushing and bumps are two doors on the same house.
Subtype matters here. ETR (erythematotelangiectatic) is mostly vascular: persistent redness, visible vessels, flushing. PPR (papulopustular) is inflammatory lesions that can look like acne. As Dr. John Barbieri at Harvard says, “The biggest mistake is treating both subtypes identically.” Most women have features of both, with one dominant.
The cascade changes how you evaluate every ingredient. Anti-inflammatories that hit NF-kB upstream (sea buckthorn, green tea EGCG) quiet the system before it spirals. Barrier-repair ingredients (ceramides, jojoba, colloidal oat) shut the door the cascade walks through. Soothing vasoactive ingredients (chrysanthemum, feverfew) calm the downstream flush.
The Ingredients Making Your Rosacea Worse Right Now
In a National Rosacea Society survey of 1,066 women with rosacea, 41% said their skincare was actively making it worse. The culprits hide in products marketed specifically to sensitive skin.
Alcohol denat topped the list at 66%. Witch hazel and fragrance tied at 30% each. Menthol hit 21%. Alcohol denat is the sneakiest of the four because it lives in toners, setting mists, “lightweight” moisturizers, and calming serums. Read labels. If alcohol denat appears in the first five ingredients of anything touching your face daily, it is working against you.
Fragrance is the next trap, and natural fragrance counts. Essential oils are not automatically safe because they are botanical. Peppermint, eucalyptus, clove, cinnamon, and citrus oils all activate TRPV1 directly, the same nerve channel from the last section. That is why a “soothing” peppermint toner can leave your cheeks scarlet for two hours.
Physical exfoliants and scrubs belong in the same bin. Dr. Sam Bunting is blunt: “Skip facials, physical scrubs, hot showers.” Anything that mechanically disrupts a fragile barrier accelerates the inflammatory chain.
Glycolic and salicylic acid at standard anti-aging strengths are too much for most active rosacea. A 10% glycolic serum on a compromised barrier is a flare waiting for a weekend. Very low-strength formulations can sometimes be tolerated, but that is a careful conversation with a dermatologist, not a guess at Sephora.
Retinol sits in an honest gray zone. Low-strength retinaldehyde in a well-buffered formula is tolerated by some rosacea-prone skin. Standard retinol in most anti-aging lines is not. If you are flaring right now, pause it and reassess in a month.
Hot water and stacking actives are the quiet accelerants. A hot shower plus vitamin C plus retinol plus an exfoliating toner delivers thermal, chemical, and mechanical insult at once. The cascade does not care that each product is “gentle on its own.”
Natural Rosacea Ingredients Worth Using
Here are the natural ingredients with meaningful evidence or mechanism for rosacea. The list starts with what you will find in Frøya’s cold-pressed formulas, then covers what else is worth knowing.
- Sea buckthorn - 26 studies confirming anti-inflammatory, antioxidant, barrier-repairing, and vascular effects. Inhibits NF-kB, JAK2/STAT1, and MAPK. Unique omega-7 content drives barrier repair at the lipid level. More on this one in the next section.
- Jojoba oil - wax ester structure closely mimics human sebum, making it uniquely compatible with barrier repair. An effective oil cleanser base and soothing carrier for active ingredients.
- Rosehip oil - rich in antioxidants and vitamin A precursors. Supports barrier function while addressing oxidative stress that runs higher in post-menopausal skin.
- Squalane - non-irritating barrier carrier derived from sugarcane or olive. Compatible with rosacea-prone skin and an ideal base for diluting sea buckthorn to the recommended 2–5%.
- Marigold (calendula) CO² extract - anti-inflammatory with a long record of use on sensitive and reactive skin. CO² extraction preserves the active flavonoids that drive the effect.
- Arctic cranberry seed oil - high in omega-3, omega-6, and tocotrienols. Antioxidant-rich, supports the barrier, and counters oxidative stress relevant to post-menopausal rosacea.
- Natural vitamin E (tocotrienols) - antioxidant that complements sea buckthorn’s carotenoid and flavonoid profile. Supports barrier function and reduces oxidative damage.
- Azelaic acid - the most clinically studied natural-origin compound for rosacea. A meta-analysis of three RCTs (N=1,624) showed 51% erythema improvement versus 36% on placebo. Five RCTs (N=2,905) confirmed strong effects for papulopustular rosacea. Naturally derived from grains, available over the counter at 10% and prescription at 15–20%.
- Mineral sunscreen (zinc oxide) - UV is a direct rosacea cascade trigger. Dr. Abby Waldman, a Harvard dermatologist who has rosacea herself, calls daily sunscreen the single most important prevention tool. Mineral rather than chemical, since chemical UV filters can provoke flushing in rosacea-prone skin.
- Niacinamide - 50-patient study showing near-complete improvement in redness, dryness, and irritation at 4 weeks. Stimulates ceramide production, rebuilding the barrier while calming inflammation.
- Chrysanthemum indicum extract - 246-patient RCT over 12 weeks with statistically significant erythema improvement (p<0.05). Useful for flushing and persistent redness.
- PD-Feverfew - the purified, parthenolide-depleted form showed a 60% reduction in IL-1alpha after UV irradiation versus placebo. A meaningful anti-inflammatory effect on one of the cytokines driving PPR.
- Colloidal oatmeal - 5-week study showed a 52% reduction in transepidermal water loss (p<0.05). A reliable barrier calmer when skin is raw and reactive.
- Green tea EGCG - anti-inflammatory and anti-angiogenic in lab models, with small topical studies showing promise for PPR.
- LED red light (630–700nm) - mechanistic support and small clinical studies. Dr. Waldman uses it 3–5 times per week on her own rosacea.
- Aloe vera, chamomile, honey - traditional use, soothing in the short term, minimal clinical data for rosacea specifically. Not harmful, just not where to focus first.
The next section goes deeper on sea buckthorn, the ingredient with the most direct overlap between the rosacea cascade and what Frøya’s formulas deliver.
Sea Buckthorn for Rosacea: What the Research Actually Shows
26 published studies confirm sea buckthorn's anti-inflammatory, barrier-repairing, and vascular effects on skin. Zero are rosacea-specific human RCTs. Both facts matter.
The mechanism map is unusually clean. Sea buckthorn inhibits NF-kB, the master inflammation switch from the cascade in the section above. It also inhibits JAK2/STAT1 and MAPK, two pathways overactive in rosacea skin. These are the precise levers rosacea pulls, and sea buckthorn pushes back on all three.
The omega-7 story sets it apart from most plant oils. Sea buckthorn seed and pulp oil are among the few botanical sources of palmitoleic acid, an omega-7 fatty acid that supports wax ester synthesis and barrier repair. Since barrier dysfunction sits upstream of the entire rosacea cascade, an oil that actively rebuilds the barrier matters more than one that just sits on top.
Vascular data backs this up. Animal and in vitro models show protective effects on small vessels, specifically relevant to the ETR subtype where visible capillaries are the complaint.
The antioxidant profile deserves attention given what you have just read about perimenopause. Sea buckthorn is unusually high in tocotrienols, carotenoids, and flavonoids. Oxidative stress drives the rosacea cascade, and post-menopause, with estrogen's antioxidant brake gone, that stress runs higher. An oil with this antioxidant density is doing useful work on that specific axis.
Practical use: 2–5% sea buckthorn oil in a squalane or jojoba base, applied at night after your moisturizer. The deep carotenoids can tint skin orange at higher concentrations, so keep the percentage modest. Especially useful for ETR where redness and vessels dominate.
Now the ingredients are sorted. Next comes building them into a routine you will stick with, which is where most rosacea advice falls apart.
A Real Natural Rosacea Routine You Can Actually Follow
If you change nothing else this week, this routine calms most rosacea-prone skin within 2 to 4 weeks. It is deliberately boring.
AM
- Gentle non-foaming cleanser with lukewarm water. Fingertips only, no brushes or cloths. Pat dry with a soft towel, do not rub.
- Azelaic acid serum, starting 2–3 times per week and building up. If azelaic acid is too much initially, use niacinamide 4–5% as a gentler alternative.
- Ceramide-based moisturizer. Look for ceramides NP, AP, and EOP, plus cholesterol and fatty acids on the label. These three together repair the barrier faster than any one alone.
- Mineral sunscreen with zinc oxide, or zinc plus titanium, SPF 30 or higher. Mineral rather than chemical, because chemical UV filters can provoke flushing in some rosacea-prone skin.
PM
- Double cleanse only if you wore makeup or sunscreen. Start with an oil cleanser (jojoba-based is ideal, since it mimics your own sebum), then follow with your gentle cleanser. On bare-skin days, use the gentle cleanser alone.
- Azelaic acid on alternate nights, or move it entirely to evening if the morning slot irritates.
- Ceramide moisturizer again.
- Sea buckthorn oil at 2–5% in a squalane base, a few drops pressed gently over the moisturizer. This step is most valuable for ETR.
Weekly
- LED red light therapy in the 630–700nm range, 10 minutes per session, 3 to 5 times per week. That is Dr. Abby Waldman’s own protocol.
- Keep a trigger journal for three weeks. Note what you ate, drank, how you slept, what you felt, and what you used on your face in the six hours before any flare. Dr. Dray points out that three weeks of honest journaling reveals most people’s top three personal triggers, often not the ones on the generic lists.
Consistency for 30 days beats any new product. If you are still flaring after a boring, consistent routine and you have addressed the hormonal piece, talk to a dermatologist.
The routine above calls for sea buckthorn oil at 2–5% in a squalane base and a jojoba-based oil cleanser. The Complete System combines both with Nordic botanicals formulated specifically for women 45+. No synthetic fragrance, no hormone disruptors, no water-based fillers.
Shop the Complete System – Save 40%When Natural Isn’t Enough: The Bridge to Clinical Treatment
Natural treatment works for a lot of rosacea, not all of it. Pretending otherwise does not help you.
The signals are concrete. Persistent pustules despite 8 to 12 weeks of a clean routine. Ocular symptoms like gritty, burning, or watery eyes, which can indicate ocular rosacea and require medical attention. Rapid worsening. Thickening of the skin on the nose (rhinophyma). As Dr. Sam Bunting says, “Rosacea is not a beauty problem, it is a medical condition.” Treat it like one when it needs to be.
Azelaic acid is the bridge ingredient between natural and clinical. It is naturally derived from grains, available over the counter at 10%, and prescription at 15–20%. It has RCT-proven efficacy (51% erythema improvement, N=1,624), and dermatologists routinely endorse it. You do not have to choose between natural and clinical when azelaic acid sits in both camps.
What a dermatologist adds that natural treatment cannot reach: topical ivermectin, which targets the Demodex-LL-37 pathway specifically. Brimonidine and oxymetazoline for rapid vascular constriction. Prescription-strength metronidazole. Oral low-dose doxycycline at sub-antimicrobial doses for severe PPR, which works as an anti-inflammatory rather than an antibiotic. IPL and pulsed-dye laser for visible telangiectasias in ETR, which no topical will erase.
The framing matters. A dermatologist’s prescription and your ceramide-sea-buckthorn-sunscreen routine are not competitors. Most dermatologists want you on a calming, barrier-repair routine underneath their prescriptions, because a healthy barrier is what makes ivermectin or metronidazole tolerable.
If your rosacea surfaced in perimenopause, ask for a dermatologist who understands hormonal skin, or coordinate with your gynecologist. They ask different questions than a generalist, and the conversation may include whether hormone therapy is appropriate, which sits outside any topical routine.