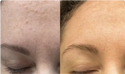
The most effective natural acne treatments for mature women are zinc (blocks DHT-driven sebum overproduction), omega-3 fatty acids (98.3% of acne patients are deficient), sea buckthorn oil (repairs the barrier while clearing pores), and gut health support (estrobolome dysbiosis recirculates acne-driving estrogen). Unlike teen acne, hormonal breakouts after 40 require barrier-safe treatments — benzoyl peroxide and strong retinoids damage ceramide-depleted skin and make things worse.
Turns out, 25% of women between 40 and 49 experience acne. This is not rare. It is barely discussed. And every natural acne treatment for mature women needs to account for what's actually happening beneath the surface.
During perimenopause, three hormonal shifts collide at once. Estrogen drops, weakening your skin barrier and slowing cell turnover. Progesterone falls, removing your body's natural anti-inflammatory protection. Testosterone's relative effect rises, driving oil production into overdrive.
This is not the same acne you had at 16. By 50, you've lost roughly 60% of your ceramides. Collagen declines at 2.1% per year after menopause. The skin you're treating now is structurally different.
That's why reaching for benzoyl peroxide or aggressive retinoids often makes things worse. Benzoyl peroxide depletes vitamin A and C from your skin, generates free radicals, and disrupts the acid mantle that's already struggling. These 10 natural treatments work with your skin's biology instead of against it. No stripping. No burning. No choosing between clearing breakouts and protecting the barrier you can't afford to lose.

1. Sea Buckthorn Oil: The Arctic Botanical That Treats Acne and Repairs the Barrier
Retinoids are the standard recommendation for both acne and aging skin. But on ceramide-depleted, collagen-reduced skin, prescription retinoids frequently cause scaling, stinging, and photosensitivity. That's not a side effect you can power through when your barrier is already compromised. Sea buckthorn offers a different path entirely.
Sea buckthorn is exceptionally rich in beta-carotene, a natural vitamin A precursor. Your body converts it to retinol at its own pace, supporting gentle cell turnover that clears clogged pores without the aggression of synthetic retinoids. This matters enormously for skin that turns over more slowly after 45.
Then there's omega-7 (palmitoleic acid), a fatty acid found almost nowhere else in the plant world. It's structurally similar to key components of human sebum, which means it repairs the lipid barrier directly and reduces transepidermal water loss.
Sea buckthorn's high vitamin C content supports collagen synthesis and brightens post-acne marks. Most women notice initial redness reduction within one to two weeks. Post-inflammatory hyperpigmentation begins fading at four to eight weeks.
2. Zinc: The Mineral That Fights Acne Like an Antibiotic (Without the Side Effects)
Most women know zinc for immune support. Few know it directly blocks the enzyme that converts testosterone to DHT, the androgen sitting at the center of sebaceous gland overactivity.
Zinc inhibits 5-alpha reductase, reducing testosterone-to-DHT conversion by approximately 30%. DHT is the primary androgen driving sebum overproduction during perimenopause. Lower DHT means less of the thick, sticky oil that clogs pores and feeds acne-causing bacteria.
Clinical trials show that 30 to 50 mg of zinc daily for 12 weeks produces results comparable to antibiotic therapy for inflammatory acne. No gut damage. No bacterial resistance. No side effects compounding on a body already navigating hormonal change.
Zinc also works as an anti-inflammatory, inhibiting NF-kB and modulating TLR2 receptors. This addresses the inflammatory cascade that makes mature skin acne more painful, more likely to scar, and slower to heal.
Zinc is not flashy. Nobody builds a brand around it. The evidence, though, is hard to argue with.
3. DIM: Shifting Estrogen Metabolism at the Source
Most articles about perimenopause acne frame it as "too much testosterone." The fuller picture: estrogen itself comes in more and less inflammatory forms. Which form your body produces matters enormously for your skin, and it's a factor almost no one talks about.
DIM (diindolylmethane), a compound derived from cruciferous vegetables, shifts estrogen metabolism toward 2-hydroxy estrone (the protective form) and away from 16-alpha-hydroxy estrone (the inflammatory, stimulating form). This reduces estrogen's own contribution to sebum production and skin inflammation, working at the metabolic level rather than the surface.
The typical dosage is 100 to 200 mg per day. Start at 100 mg. Full benefits for hormonal acne take two to three months, so this requires patience.
The evidence for DIM is promising but still emerging. It is one piece of a hormonal puzzle, not a complete solution on its own.
4. Omega-3 Fatty Acids: The Deficiency Almost Every Acne Patient Shares
A 2024 study in the Journal of Cosmetic Dermatology found that 98.3% of acne patients had omega-3 deficits at baseline. Acne severity correlated directly with the degree of deficiency. That number is worth sitting with.
Omega-3s (EPA and DHA) work through a triple mechanism. They reduce sebum synthesis at the gland level, lower inflammatory cytokines systemically, and decrease androgen-driving hormones. This directly counters the relative androgen dominance of perimenopause. Fish oil specifically has been shown to reduce serum testosterone in women.
EPA is the primary anti-inflammatory, responsible for reducing the prostaglandins that drive acne-related redness and swelling. DHA supports skin barrier integrity at the cellular level. Both matter, and most women are deficient in both.
The benefits extend beyond skin: cardiovascular protection, mood stabilization, joint support. For women in midlife, omega-3 supplementation serves multiple needs simultaneously, making it one of the most efficient additions to any protocol.
If you do one thing from this entire list, correcting an omega-3 deficit may be the single highest-return intervention you can make.
5. Gut Health: Why Your Skin Reflects What Happens Below the Surface
"Your skin is a mirror. It's a reflection of your gut health." A triple board-certified OB/GYN put it that plainly, and it reframes why topical-only approaches so often fail.
Your gut houses a specific collection of bacteria called the estrobolome, and these bacteria metabolize estrogen. When gut flora is disrupted, excess estrogen recirculates through your body instead of being properly excreted. This worsens hormonal acne from the inside, through a pathway that no cream or serum can reach.
Consider that 70% of your immune system lives in your gut. When dysbiosis takes hold, it generates systemic inflammation that shows up on your skin. On a mature barrier already sensitized by hormonal change, that inflammation hits harder and heals slower.
Here's what actually helps. Add diverse-strain probiotics (particularly Lactobacillus strains) and fermented foods like sauerkraut and kimchi. Support your liver's hormone detox capacity with milk thistle and dandelion root tea. Reduce dairy and high-glycemic foods. Dr. Tabatha recommends an eight-week elimination of sugar, dairy, and gluten to identify your triggers.
If breakouts persist despite topical and dietary changes, consider a functional stool test. Dr. Terry Loong, a skin and hormone specialist who struggled with perimenopausal acne herself, credits gut dysbiosis treatment as the intervention that finally cleared her skin.
6. Rosehip Oil: Fading the Dark Marks Acne Leaves Behind
At 25, a pimple mark fades in weeks. At 50, the same mark can linger for six to 12 months. Reduced cell turnover, less collagen, more inflammation sensitivity. Post-inflammatory hyperpigmentation on mature skin is a fundamentally different problem: epidermal PIH can persist six to 12 months, while dermal PIH can last years.
A clinical study of 108 adults found that rosehip oil applied twice daily produced significantly better scar appearance scores (less erythema, discoloration, and atrophy) at six to 12 weeks compared to no treatment. Rosehip is rich in polyphenols with antioxidant action and vitamin E for anti-inflammatory support.
There's another layer. Acne-prone skin is characteristically deficient in linoleic acid, which makes sebum thicker and more likely to oxidize and clog pores. Rosehip oil is linoleic-rich, correcting this deficiency at the barrier level. It treats current breakouts while fading past ones.
7. Tea Tree Oil: How to Use It Safely on Mature Skin
Tea tree oil is probably the first natural acne remedy you've ever heard of. It works. The question for mature skin is how to use it without triggering irritation on a barrier already running thin.
Tea tree oil is clinically proven as both antibacterial and anti-inflammatory, with studies showing it comparable to benzoyl peroxide for mild acne, with fewer side effects. But there's a significant sensitization risk when applied undiluted, especially on ceramide-depleted skin. The line between therapeutic and irritating is narrower than most people realize.
Safe dilution for mature skin: two drops of tea tree oil in 12 drops of jojoba oil (a carrier that won't clog pores). Apply as a spot treatment only, not all-over. This delivers the antibacterial benefit precisely where you need it without compromising the surrounding barrier.
If even diluted tea tree feels too aggressive, manuka essential oil (diluted to 1%) kills acne bacteria without the same sensitization risk. Less studied, but gentler.
Tea tree is a scalpel, not a sledgehammer. Precision matters more on mature skin.
8. Jojoba Oil: The Counterintuitive Sebum Regulator
Putting oil on acne-prone skin sounds exactly wrong. But jojoba oil is not really an oil. It's a liquid wax ester, structurally almost identical to human sebum.
Jojoba's molecular structure mimics sebum so closely that it signals your sebaceous glands to reduce their own oil production. This is the opposite of what happens when you strip your skin with harsh cleansers or drying acne treatments, which trigger compensatory overproduction.
Your skin panics when its barrier is compromised. It floods itself with more oil (or thicker oil) trying to repair the damage. Supporting the barrier with sebum-mimicking oils breaks that cycle. Dr. Terry Loong, who dealt with perimenopausal breakouts personally, describes this exact mechanism.
Jojoba is non-comedogenic, anti-inflammatory, and an excellent carrier for tea tree oil dilution (connecting back to the spot treatment in the previous section).
Sometimes the best way to control oil is to stop fighting it.
9. Vitex (Chasteberry): Herbal Hormone Support for Perimenopause
If your cycles are still showing up (even erratically), there's an herb with centuries of traditional use and modern clinical backing for the hormonal chaos of perimenopause.
Vitex agnus-castus acts on the pituitary gland to regulate luteinizing hormone (LH) and prolactin, smoothing the hormonal fluctuations that drive cyclical breakouts. When your hormones swing wildly from month to month, your skin reacts. Vitex helps reduce that swing.
An eight-week randomized controlled trial showed significantly lower menopausal disorder scores, anxiety levels, and vasomotor symptoms in the vitex group versus placebo. No serious adverse events were reported. A separate clinical study found that chasteberry eliminated or improved menstrual-related acne.
Vitex is most appropriate during perimenopause, when cycles are still present. Post-menopause, when ovarian hormone production has essentially ceased, its mechanism is less clear and its usefulness less certain.
Vitex is not for everyone. But for perimenopausal women whose breakouts track with their cycle, it addresses a specific hormonal gap that topical treatments cannot touch.
10. Stress, Cortisol, and the Adaptogen Question
Perimenopause does not arrive in a vacuum. It shows up alongside career pressure, aging parents, teenagers, and sleep disruption. That stress is not abstract. It is biochemical. And it shows on your skin.
Cortisol drives acne independently of sex hormones. Elevated cortisol increases sebum production, impairs wound healing, and weakens the skin barrier. Stress also worsens gut health, creating a vicious cycle through the gut-brain-skin axis (connecting directly back to the gut health section above).
Ashwagandha is the most popular adaptogen for cortisol reduction, and studies show it can lower cortisol by up to 32%. But here's a critical caveat: ashwagandha also raises testosterone by approximately 15% and DHEA-S by approximately 18%. For women already dealing with relative androgen dominance, ashwagandha can worsen the exact hormonal pattern driving acne. The cortisol goes down. The breakouts get worse.
Or skip the supplement aisle entirely and focus on non-supplement cortisol management: sleep hygiene (seven to nine hours consistently), regular movement, and the gut-reset protocol covered earlier.
Managing cortisol is not optional in midlife. The method matters. Not every popular supplement fits every woman's hormonal profile.