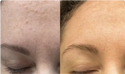
Menopause skin changes happen because estrogen decline rewires your skin at every level - barrier integrity, pH balance, collagen production, oil output, and inflammatory response. In perimenopause, erratic estrogen fluctuation makes these shifts unpredictable, which is why products that worked for years can suddenly cause burning, stinging, or simply stop delivering results. These changes can begin as early as your late 30s, years before a formal menopause diagnosis.
This article covers the eight specific changes most responsible for that breakdown - the science driving each one and what actually helps, including plant-based alternatives most dermatology resources never mention.
1. Collagen Loss Accelerates Faster Than You Think
Here is a number that stopped me cold: your skin loses up to 30% of its collagen in the first five years after menopause. Nearly a third of your skin’s structural scaffolding, gone in the time it takes to blink through early menopause.
Estrogen directly stimulates fibroblasts, the cells responsible for producing collagen. When estrogen declines, those fibroblasts slow down. Cortisol compounds the damage. Research published in Science (2025) shows that cortisol activates matrix metalloproteinases (MMPs), enzymes that digest existing collagen, while simultaneously suppressing new collagen synthesis. Stress plus menopause equals a double hit. After that initial 30% drop, you lose roughly 2% per year for the next 20 years.
I need to be honest about retinol. Yes, it stimulates collagen. But on thinning, sensitized menopausal skin, retinol frequently causes peeling, redness, and stinging. A 2019 randomized controlled trial published in the British Journal of Dermatology found that bakuchiol, a plant-derived compound, delivered comparable improvements in wrinkles and hyperpigmentation with significantly fewer side effects. A 2025 network meta-analysis in Scientific Reports confirmed those findings.
Rosehip oil delivers the same collagen-supportive nutrients without the irritation. It is rich in natural vitamin A (beta-carotene and retinol esters), vitamin C, and linoleic acid, in a form that sensitive menopausal skin handles well.
2. Your Skin Barrier Is Losing Its Armor
“Skin so dry not even body butter helps.” If that sounds like you, the problem is not hydration. It is your barrier.
Your skin’s acid mantle normally sits at a pH of 4.5 to 5.5. Menopause shifts that pH toward alkaline. This matters because an enzyme called acid sphingomyelinase needs that acidic environment to produce ceramides. Ceramides make up roughly 50% of your barrier lipids, so fewer ceramides means barrier collapse.
Estrogen decline also reduces the fatty acids and cholesterol in your barrier. The result is increased transepidermal water loss (TEWL). Water escapes your skin faster than you can replace it.
This is exactly why water-based moisturizers fail so many women at this stage. Most mainstream moisturizers are 60 to 80% water. On a compromised barrier, that water evaporates, and it takes your skin’s own moisture with it.
Oil-based and waterless formulas work differently. They act as occlusives, physically reducing TEWL by sealing the barrier. Think of it as putting a lid on a pot of boiling water versus spraying more water into the steam. One stops the loss. The other adds to the chaos.
The best strategy is a two-step approach. Apply a humectant-rich serum first (rosehip or sea buckthorn oil draws moisture in), then follow with an oil-based layer that locks it there. Your barrier needs sealing, not just soaking. That is the difference between temporary relief and real repair.
3. The Itch That Nobody Warned You About
Kate Hartley described it as “invisible lice all over your skin.” Itching is one of the most common menopause skin changes, and one of the least discussed.
Research published in PNAS (2021) shows that estrogen modulates itch through the spinal GRP/GRPR system. When estrogen declines, that regulatory pathway weakens. A 2023 review in PMC identified a bidirectional histamine-estrogen disruption: falling estrogen amplifies histamine activity, and elevated histamine further disrupts estrogen signaling.
During perimenopause, when estrogen fluctuates rather than steadily declining, the itch can be erratic. It comes and goes without pattern, which makes it easy to dismiss as dry skin or allergies. Barrier collapse compounds the problem. A compromised barrier means nerve endings sit closer to the surface, more exposed to irritants. Two systems failing at once.
What helps in practice: itching worsens in dry winter months, so run a humidifier in your bedroom. Histamine-rich foods can intensify it (aged cheese, fermented foods, alcohol, tomatoes, and avocado). Oatmeal baths and lukewarm water (never hot) soothe without stripping. And fragrance in skincare acts as an itch trigger on a compromised barrier.
4. Inflammaging Is Why Your Skin Overreacts to Everything
Your favorite serum did not change. Your skin did. If products that worked for a decade now sting, flush, or cause breakouts, there is a name for what is happening: inflammaging.
Inflammaging is chronic, low-grade inflammation driven by hormonal decline. It shows up as flushing, rosacea flares, and heightened reactivity to ingredients your skin previously tolerated. Thinner skin from collagen loss combined with a compromised barrier means less buffer between irritants and nerve endings. Your skin’s shifted pH is why products you have used for years can suddenly cause burning or stinging. This is not sensitivity you developed. It is inflammation your body can no longer suppress.
Here is where many women make it worse. The instinct is to add more products. Stylist Magazine put it directly: “Skincare overloading is not a smart solution to hormone issues.” Facial plastic surgeon Dr. Amir Karam advocates “fewer, better products” over stacking actives on reactive skin. Each new active ingredient is another potential trigger on an already inflamed canvas.
Fragrance-free, minimal-ingredient formulas reduce the trigger load. Cold-pressed botanical oils contain fewer synthetic compounds to react to. The approach that works is counterintuitive: simplify before you add. The Instant Rosacea, Acne & Redness Stopper follows exactly this philosophy, using only ingredients you can verify on our Ingredients page.
5. Hormonal Acne and Dryness Can Happen at the Same Time
Acne products strip the oil you desperately need. Moisturizers clog the pores that are already breaking out. Sound familiar?
Perimenopause means fluctuating, not steadily declining, estrogen. One week, estrogen drops, your skin dries out, and your barrier weakens. The next week, relative androgen excess (estrogen drops but androgens stay stable) triggers sebum overproduction. The result: an oily T-zone, flaking cheeks, and hormonal cystic acne along the jawline. This is not teenage acne and should not be treated the same way.
Conventional acne products backfire here. Salicylic acid and benzoyl peroxide are drying agents that further compromise an already weakened barrier. Stripping cleansers push your pH further alkaline, making everything worse.
Start with a gentle, pH-balanced cleanser instead. Use lightweight plant oils like rosehip, which is rich in linoleic acid, non-comedogenic, and actually helps balance sebum production. Treat the barrier first, acne second. Your skin is not confused. Your hormones are sending mixed signals, and your routine needs to account for both.
6. Hormone Disruptors in Your Skincare Are Making It Worse
The moisturizer on your nightstand might contain ingredients that mimic estrogen. During menopause, that is the last thing your body needs.
Parabens are estrogenic. They bind to estrogen receptors in your body. Phthalates interfere with hormone signaling. Research confirms topical absorption of both. A 2025 study published in Frontiers in Reproductive Health found that menopausal women are disproportionately sensitive to endocrine-disrupting chemicals (EDCs). When your endocrine system is already in flux, adding synthetic hormone mimics creates unpredictable effects.
Here is what to look for on labels. Parabens appear as methylparaben, propylparaben, and butylparaben. Phthalates are often hidden under the word “fragrance,” which manufacturers are not required to disclose as individual compounds. A single synthetic fragrance listing can contain dozens of undisclosed chemicals. You could be applying endocrine disruptors nightly without any way to know from the label alone.
Cold-pressed plant oils do not contain hormone-disrupting compounds. Waterless formulas eliminate the preservatives needed to stabilize water-based products. Fewer ingredients means fewer unknowns entering your body through your skin. This matters more during menopause than at any other stage, because your endocrine system has less capacity to compensate for outside interference.
| Avoid | Choose Instead |
|---|---|
| Foaming soaps (pH 9–10) | Low-pH gel cleanser (pH 5–6) |
| Water-based creams (60–80% water) | Occlusive oil balm (waterless) |
| Synthetic fragrance / parfum | Fragrance-free formulas |
| Parabens, phthalates | Cold-pressed plant oils |
| Retinol (irritating on reactive skin) | Rosehip oil / bakuchiol |
Read your labels. If you cannot identify an ingredient, research it before you put it on your face. You can see exactly what goes into every Froya product on our Ingredients page, and the research behind our formulations on our Science page.
7. Your Cleanser Might Be Your Biggest Problem
Before you buy another serum, look at what you are washing your face with.
High-pH cleansers (soaps and foaming washes) typically sit at a pH of 9 to 10. Healthy skin pH is 4.5 to 5.5. Menopause is already pushing your pH toward alkaline. Using a high-pH cleanser on top of that creates a double disruption. Remember acid sphingomyelinase, the ceramide-producing enzyme? It needs an acidic environment to function. Every wash with the wrong cleanser actively degrades your barrier.
The swap is simple but high-impact. Choose a non-foaming, fragrance-free, low-pH cleanser. If it lathers aggressively, it is probably too harsh. This single change can improve how every other product in your routine performs, because a functioning barrier absorbs and retains actives more effectively. Your expensive serums cannot do their job if your cleanser destroys the surface they need to penetrate.
If your skin feels tight after washing, your cleanser is the problem. That tight feeling is not “clean.” It is stripped lipids and moisture loss. If you already use a gentle, non-foaming cleanser, you are ahead of most. For gentle exfoliation that respects your barrier’s pH, try the Ultra Cleanse & Revive Face Scrub.
8. A Menopause Skincare Routine That Actually Works
Dr. Onikepe Adegbola, MD PhD, said it clearly: “Women deserve better than being told it is just aging.” I agree. Here is a routine built for what your skin actually needs right now.
Morning:
- Gentle, pH-balanced cleanser with lukewarm water (not hot)
- Lightweight plant oil or serum. Rosehip oil or sea buckthorn oil are ideal. Sea buckthorn delivers omega-7 and over 190 bioactive compounds.
- Occlusive balm to seal your barrier, like the Anti-Age & Insane Glow Day Balm
- SPF. Non-negotiable. Thinner skin means more UV damage penetrates deeper.
Evening:
- Same gentle cleanser
- A natural vitamin A treatment. Rosehip delivers retinol-equivalent compounds (beta-carotene, retinol esters) alongside vitamin C and linoleic acid for collagen support without irritation. The Magic Wrinkle Eraser Night Balm uses rosehip and marigold for overnight repair.
- Rich occlusive balm or night balm to support overnight repair
Weekly:
- Gentle exfoliation one to two times per week. Not daily. Not harsh scrubs.
Lifestyle:
- Omega-3 rich diet to support barrier function from the inside
- Reduce histamine-triggering foods if you experience itch or flushing
- Humidifier in winter to counter seasonal dryness
- Stress management matters. Cortisol degrades collagen.
The philosophy behind this routine comes from Dr. Amir Karam’s principle: fewer, better products. Barrier repair is the foundation. Oil-based and waterless products reduce TEWL more effectively than water-based alternatives. Sea buckthorn, supported by clinical trial NCT00767156, delivers 190+ bioactive compounds that nourish without irritating.
Start with the cleanser swap and an occlusive balm. Build from there.

Ready to Build Your Routine?
The Complete System for Mature Women’s Skin includes everything in this guide - formulated around your biology.
Shop the Complete SystemFree UK delivery · 30-day returns · No synthetics